Understanding Menopausal Symptoms and the Role of Hormone Therapy
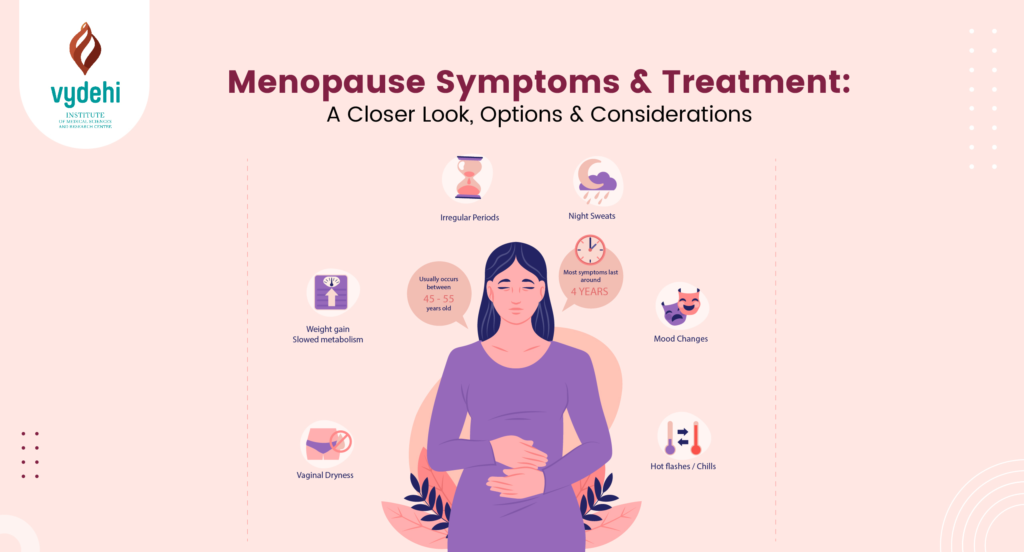
Search Phrase: Menopause hormone safety plays a crucial role in how women experience this natural life transition. Menopause marks the end of menstrual cycles and is often accompanied by bothersome symptoms such as hot flashes, night sweats, mood swings, vaginal dryness, and sleep disturbances. These symptoms are primarily caused by a decline in estrogen levels as the ovaries reduce hormone production (source).
Many women turn to hormone therapy (HT), especially estrogen therapy, which is widely recognized for its ability to alleviate menopausal symptoms effectively. Estrogen helps restore hormonal balance, reducing the frequency and severity of hot flashes and night sweats, improving mood, and supporting vaginal and urinary tract health. Beyond symptom relief, HT also offers protection against osteoporosis by slowing bone loss that accelerates post-menopause (source).
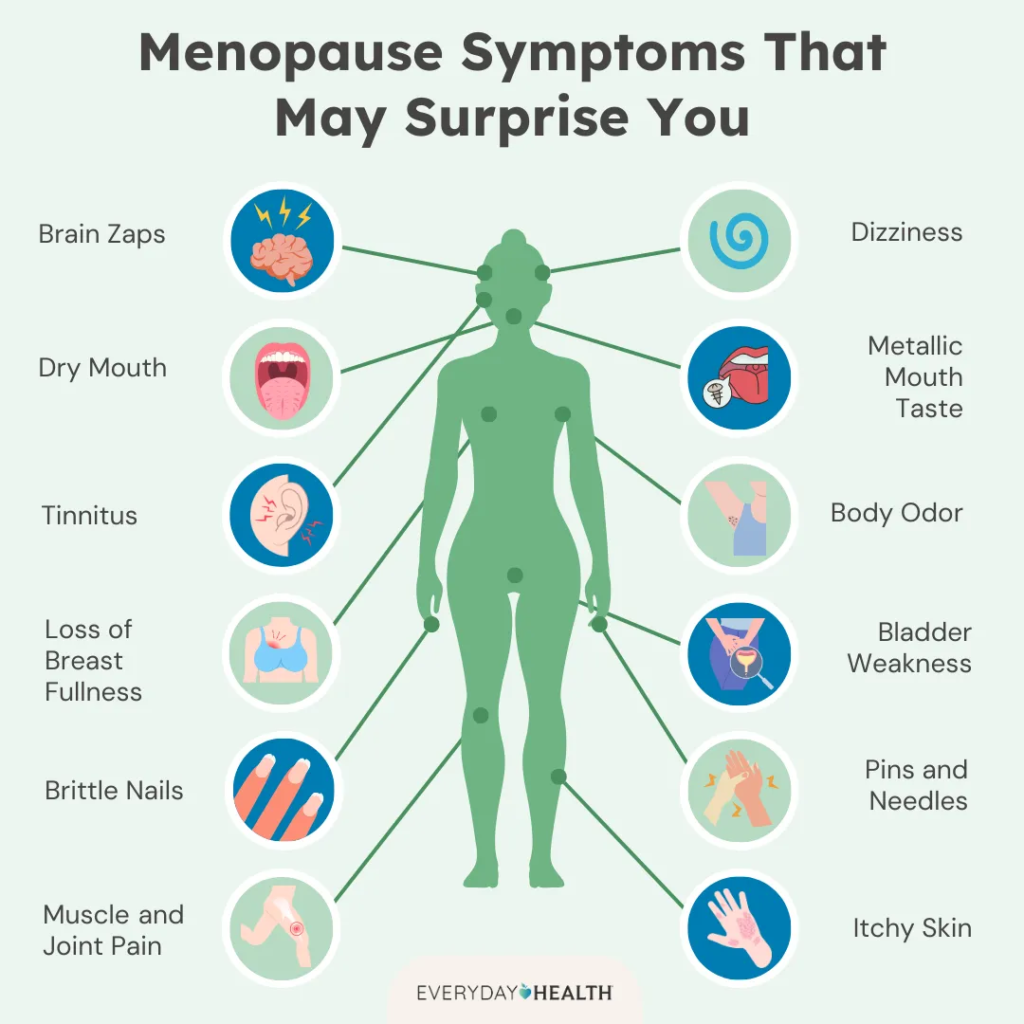
However, discussions about menopause hormone safety often surface due to concerns about potential risks. Research indicates that for many women—particularly those beginning hormone therapy near menopause onset—the benefits surpass the risks. The safety of hormone therapy depends on various factors, including the type of hormones used, delivery method (patches, pills, gels), dosage, treatment duration, and individual health circumstances (source).
Women considering hormone therapy should consult healthcare providers to personalize their treatment plans. It’s also beneficial to explore complementary approaches such as lifestyle modifications and natural remedies—read more about these in our article 7 Effective Strategies to Embrace Healthy Aging and Thrive.
Understanding the Black Box Warning on Menopause Hormone Therapy: Meaning and Implications
A black box warning is the FDA’s most serious alert indicating potential severe risks associated with a medication. For menopause hormone therapy (MHT), this warning highlights concerns about increased risks of heart disease, stroke, blood clots, and breast cancer linked to certain hormone treatments (source).
This warning originated after large studies like the Women’s Health Initiative (WHI) revealed increased cardiovascular and cancer risks, particularly in women who started therapy many years after menopause. Yet, current understanding emphasizes the importance of a personalized risk assessment—considering factors like age, health history, and hormone formulations (source).

It’s vital for women to discuss their medical background thoroughly with healthcare providers. Adjustments such as lower doses, shorter duration, or estrogen-only therapy (for women without a uterus) may mitigate some risks. Additionally, non-hormonal options and lifestyle changes are practical alternatives. While the warning underscores caution, it does not mean hormone therapy is unsafe for all; rather, safe use involves careful, individualized evaluation (source).
Who Benefits from Menopause Hormone Safety and Who Should Be Cautious
Research indicates that hormone therapy can be highly effective, especially when started within 10 years of menopause or before age 60—known as the “timing hypothesis.” This approach helps optimize benefits while minimizing risks concerning cardiovascular health and bone density preservation (source).
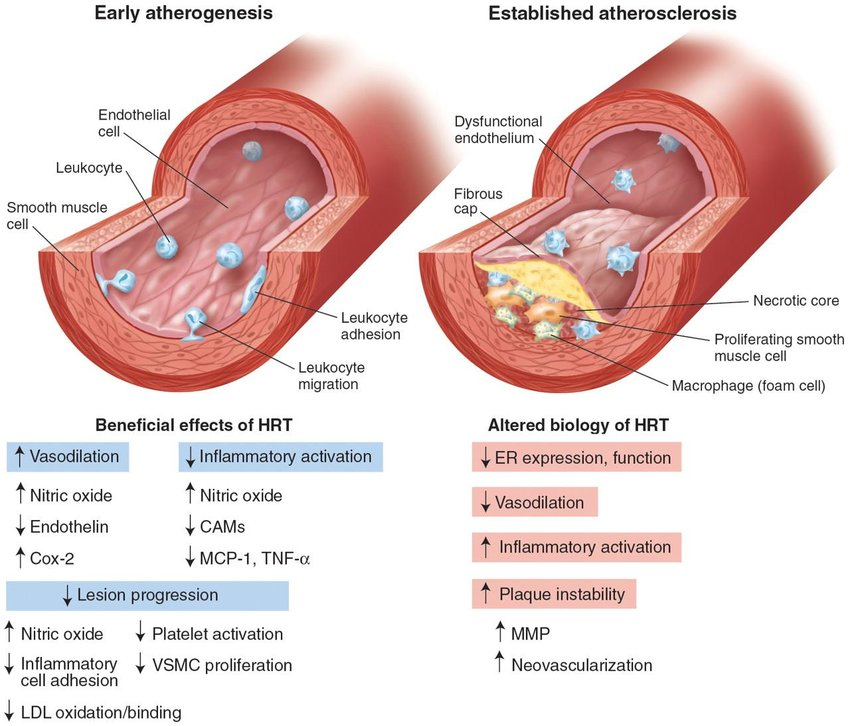
Women most likely to benefit are those experiencing moderate to severe symptoms affecting their daily life or those at high risk for osteoporosis. Estrogen therapy reduces fracture risk and can even improve mood and cognitive function in some cases. Nonetheless, a detailed individual assessment—including personal and family health history—is essential before starting treatment.
On the other hand, hormone therapy is generally contraindicated for women with a history of breast cancer, unexplained vaginal bleeding, liver disease, blood clots, or stroke. The risks tend to increase with age and longer use, so ongoing monitoring by healthcare professionals is critical to ensure safety and efficacy (source).
Women should also consider non-hormonal options and lifestyle adjustments—such as diet, exercise, and stress management—to manage symptoms safely and holistically. Open dialogue with healthcare providers helps tailor the most appropriate and safe approach (source).
Future Directions in Menopause Treatments and Safety Innovations
Emerging treatments focus on addressing menopause symptoms effectively while ensuring menopause hormone safety. For instance, bioidentical hormone replacement therapies (BHRT) are designed to closely match the body’s natural hormones, aiming to reduce associated risks of traditional hormone therapy by offering more personalized dosing and administration routes (source).
Additionally, non-hormonal therapies such as SSRIs, non-hormonal pharmacologic agents, and targeted nerve stimulation are gaining recognition for their efficacy in alleviating hot flashes and mood swings. Complementary methods like diet, supplements, and mind-body techniques are increasingly validated through clinical research to provide safe symptom relief (source).
Innovations in delivery systems—like transdermal patches or vaginal rings—are designed to optimize hormone absorption with fewer systemic side effects, further enhancing safety profiles. Ongoing genetic and molecular research aims to customize treatments based on individual risk factors, opening new horizons in menopause management (source).
For women seeking natural options, research into phytoestrogens and plant-based compounds continues to explore their potential efficacy and safety. Staying informed about advances in menopause hormone safety ensures women can make choices aligned with their preferences and health needs (source).
How to Discuss Menopause Hormone Safety with Your Healthcare Provider
Effective communication with your healthcare provider is vital for understanding and managing menopause hormone safety. Here are some key tips to guide your discussions:
- Prepare Ahead: Before your appointment, list your symptoms, concerns, medical history, and questions about menopause hormone safety. Include details about family history, current medications, and previous treatments (source).
- Understand Risks and Benefits: Ask your provider to explain the benefits of hormone therapy and potential risks such as cardiovascular issues or cancer. Clarify how these relate to your age, health status, and therapy duration (source).
- Explore Alternatives: Inquire about non-hormonal options like lifestyle modifications, supplements, or alternative therapies, so you can make an informed decision that aligns with your comfort and safety.
- Bring a Support Person: Having a trusted friend or family member attend can help you remember important details and provide emotional support during your discussion.
- Request Written Information: Ask for educational materials to review at home. These will help reinforce your understanding of menopause hormone safety and aid in follow-up conversations.
- Plan for Follow-up: Establish regular check-ins to monitor symptoms, side effects, and treatment effectiveness, emphasizing that managing menopause safely is an ongoing process (source).
Dispelling Myths and Exploring Natural Alternatives in Menopause Hormone Safety
Many misconceptions surround menopause hormone safety. Outdated studies and generalized fears have led to unnecessary apprehension about hormone replacement therapy (HRT). In reality, when prescribed and monitored carefully, HRT remains a safe, effective option for symptom relief and osteoporosis prevention (source).

A common myth is that HRT significantly increases breast cancer risk. Current evidence suggests this risk is multifaceted and depends on factors like hormone type, dosage, and duration. Bioidentical hormones, which mimic the body’s natural hormones, are garnering attention as potentially safer options, though long-term safety data are still emerging (source).
Additionally, lifestyle modifications—such as regular exercise, a balanced diet rich in phytoestrogens (e.g., soy, flaxseed), stress reduction, and supplements—offer effective symptom management without hormones. Emerging therapies, including nerve stimulation and cognitive-behavioral techniques, provide additional avenues for relief.
Understanding menopause hormone safety is heavily reliant on personalized consultation with healthcare providers. Staying informed about the latest research ensures women can make empowered, safe choices during this transition (source).
Sources
- WellnessBlogs – 7 Effective Strategies to Embrace Healthy Aging and Thrive
- FDA – WHI Study and Hormone Therapy Warning
- Mayo Clinic – Menopause and Hormone Therapy
- NHS – Menopause Hormone Therapy Safety and Benefits
- National Heart, Lung, and Blood Institute – Hormone Therapy and Menopause
- National Library of Medicine – Hormone Therapy and Risks
- Additional Insights on Healthy Aging
- WellnessBlogs


