Understanding Cannabis Use Disorder: Rising Concerns in a Changing Legal Landscape
Search Phrase: Varenicline cannabis highlights a growing health concern amidst the changing legal status of cannabis worldwide. Cannabis Use Disorder (CUD) is a condition characterized by problematic cannabis consumption that leads to significant impairment or distress. As legalization expands, the prevalence of CUD has increased, prompting public health officials and researchers to seek effective treatment options [source].
While many cannabis users do not develop dependence, approximately 9% may experience symptoms such as cravings, withdrawal, and continued use despite adverse consequences [source]. The health effects of CUD are multifaceted, impacting mental health through heightened anxiety, depression, or psychosis in vulnerable individuals, and impairing cognitive functions like memory and attention. Socially, individuals with CUD often face challenges in their occupational and personal lives, which can contribute to broader societal issues [source].
With increasing accessibility of cannabis due to legal reforms, there is an urgent need for effective treatment strategies. One promising approach is the use of varenicline, a medication primarily used for smoking cessation, which has shown potential in reducing cannabis use and cravings [source]. Understanding how varenicline works can provide valuable insights into managing CUD in the context of legal and recreational cannabis use.
Varenicline: A Promising Aid for Cannabis Use Reduction
Search Phrase: Varenicline cannabis is increasingly being studied for its role in managing cannabis dependence. Originally developed to target nicotine addiction by acting on nicotinic acetylcholine receptors in the brain, varenicline’s mechanism of action may extend to other substances, including cannabis [source].
Neurochemical Pathways and Its Effects
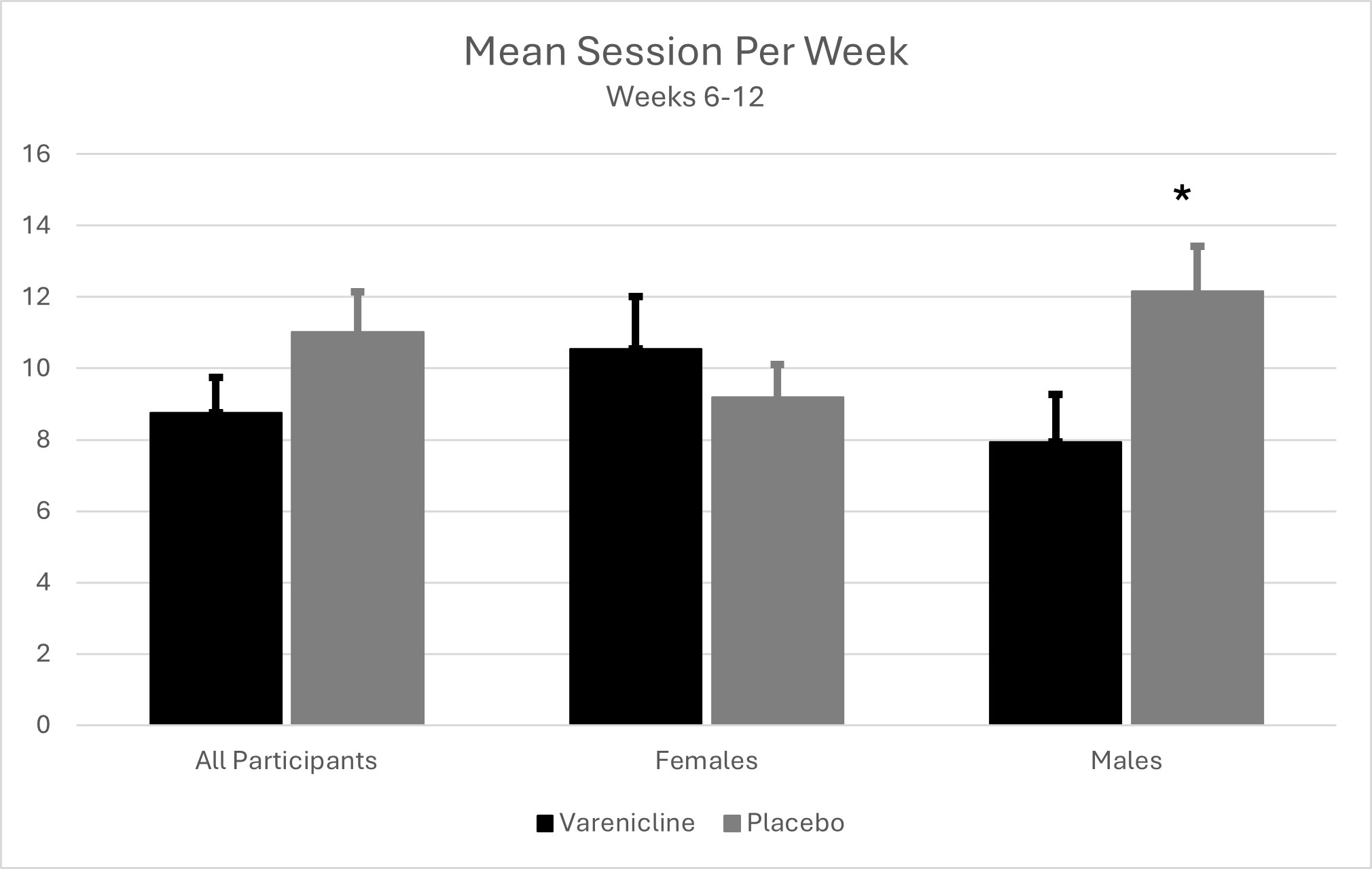
Research suggests that varenicline functions as a partial agonist, which can diminish the rewarding sensations associated with cannabis use. This, in turn, can help decrease cravings and withdrawal symptoms, facilitating cessation efforts [source]. Clinical trials indicate that varenicline may reduce the frequency and intensity of cannabis use, making it a potentially significant pharmacotherapy in CUD treatment [source].
Potential Benefits and Limitations
While the preliminary data are promising, the application of varenicline for cannabis dependence is still being explored. Its ability to mitigate withdrawal-related irritability and anxiety without the adverse effects seen in some other medications makes it an attractive candidate [source]. Nonetheless, more research is necessary to confirm long-term safety and optimal dosing regimens [source].
Recent Clinical Insights into Varenicline for CUD Treatment
Search Phrase: Varenicline cannabis is at the forefront of recent clinical investigations aimed at broadening the therapeutic landscape for CUD. Such studies have demonstrated that Varenicline significantly reduces cannabis cravings and use, especially among individuals motivated to quit [source].
Clinical Trials and Outcomes
Emerging data from clinical trials show that Varenicline decreases both the frequency and amount of cannabis consumed, supporting its potential as an effective pharmacological option [source]. This is particularly relevant because few FDA-approved treatments currently exist for CUD, raising expectations for Varenicline’s integration into standard care protocols [source].
Implications for Treatment Strategies
Integrating medications like Varenicline with behavioral therapies can offer a comprehensive approach to CUD. Combining pharmacology with counseling improves the odds of achieving and maintaining abstinence while managing withdrawal symptoms effectively [source]. This multi-modal approach is critical as the field moves toward more personalized addiction care.
Future Directions and Considerations
Search Phrase: Varenicline cannabis continues to be a focus of ongoing research that promises to refine and enhance treatment options for CUD. As studies advance, there is hope that dosing protocols will be optimized, safety profiles clarified, and regulatory approval obtained for wider clinical use [source].
The expanding scientific understanding underscores the importance of integrating new pharmacotherapies with holistic mental health and behavioral strategies [source]. Staying informed about these developments can help practitioners provide more effective, evidence-based care for individuals struggling with cannabis dependence.