Understanding the Obesity Prevalence in the U.S.: A Deep Dive
Search phrase: obesity prevalence in the U.S.
The obesity prevalence in the US is a major concern for health officials, providers, and policymakers. As a health expert, I’ve seen how these numbers reflect societal changes and affect Americans’ well-being across all ages. Obesity rates have soared over the past fifty years. This increase affects physical health, raises healthcare costs, and lowers quality of life. This article looks at trends in obesity, what causes it, its effects, and ways to tackle the problem.
Historical Trends in Obesity: From the 1970s to Today
The obesity prevalence in the US has increased by a large margin since the 1970s. In the early 1970s, researchers classified about 15% of American adults as obese. By the late 1990s, this figure had more than doubled, with the CDC reporting over 30% of adults classified as obese. Today, estimates show that obesity rates exceed 40%, highlighting a public health crisis. For more details, see the CDC data on obesity prevalence.
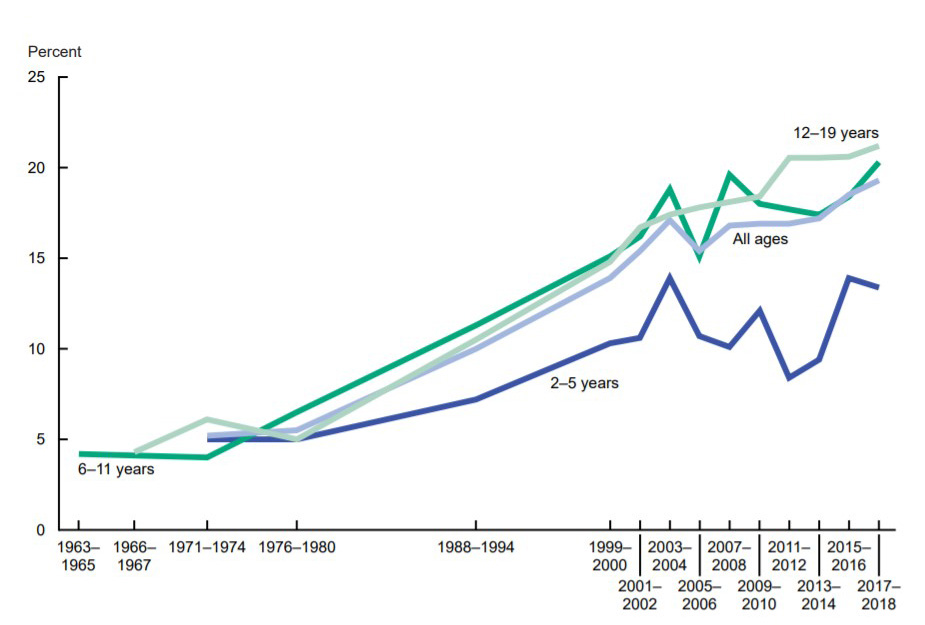
Children are not exempt from this trend. In 1971–1974, roughly 5% of children were obese. Alarmingly, data from 2017–2020 show that nearly one in five children is now obese, raising concerns about chronic disease risks. Many factors have played a role. These include more processed food, less physical activity, urban living, and economic differences. From my experience working with children in health programs, I’ve seen how habits form early and how hard they can be to change.
Understanding these trends helps us see the complex nature of obesity in the U.S. today. Efforts to fight this epidemic now focus on big changes. These include community programs, policy updates, and actions by individuals. For example, promoting physical activity and healthy eating from a young age is essential. For practical insights, see our article on the benefits of physical activity.
Understanding Severe Obesity: What the Numbers Reveal
While general obesity rates are high, severe obesity—defined as a BMI of 40 or higher—is rising even faster. This extreme weight poses serious health risks. These include type 2 diabetes, heart disease, some cancers, and a higher risk of death. The CDC says severe obesity has almost doubled in the last 20 years. This rise adds a lot of stress to healthcare systems. Learn more about severe obesity at the CDC on chronic diseases.
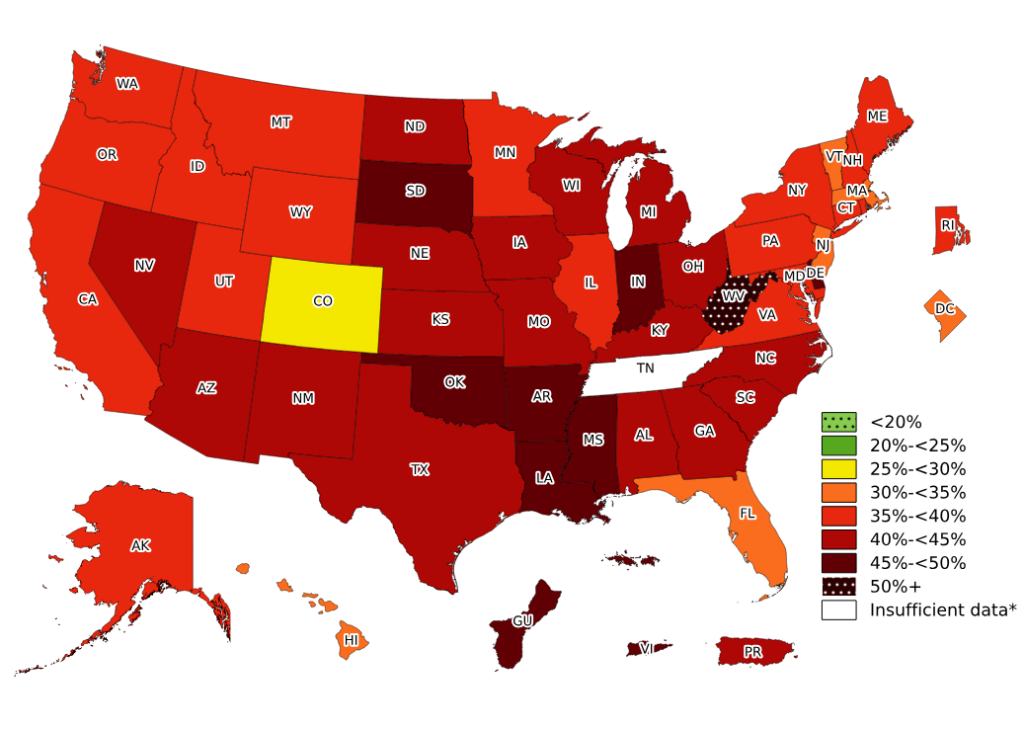
The increase in severe obesity means more Americans face health-threatening weight levels. I’ve worked with patients facing severe obesity. Their care often includes treatments like behavioral therapy and, at times, surgery. Recognizing this trend highlights the need for early intervention and tailored treatment plans.
Understanding obesity in the US is crucial. The increase in severe cases calls for strong public health actions. Lifestyle factors, such as a bad diet and lack of exercise, mix with genetics and social influences. So, targeted strategies are essential. For those interested in how lifestyle changes can impact health, see our article on lifestyle risk factors.
Factors Contributing to the Obesity Epidemic
Lifestyle and Behavioral Factors
The obesity prevalence in the US is heavily influenced by lifestyle choices. Sedentary behavior, increased screen time, and reduced physical activity are key factors. A shift from active outdoor play to desk jobs has led to an energy imbalance—more calories in than out. Many clients struggle to find time or motivation for exercise, reflecting broader societal trends.
Dietary Patterns and Food Environment
The rise of processed foods and fast food culture has worsened the issue. Many low-income communities face limited access to affordable, nutritious food. This is called a “food desert.” As a result, they often rely on high-calorie, low-nutrient foods. Socioeconomic disparities worsen obesity rates among vulnerable groups. Environmental factors play a big role. Cities that don’t encourage walking make things harder. There are also fewer places for recreation. For more on dietary patterns, see the USDA on dietary patterns.
Understanding these factors shows that tackling obesity requires more than individual responsibility. It needs systemic changes in community design and food marketing. For insight into how the environment affects health, check our article on the benefits of parks.
Economic and Cultural Influences
Economic conditions matter too. Lower-income communities have problems. They struggle with limited healthcare access. They also face higher stress levels. Cultural norms about diet and activity also shape behaviors. As a healthcare professional, I’ve noticed that cultural attitudes can support unhealthy habits if we don’t handle them carefully.
Impacts of Obesity on Public Health and Healthcare Systems
The obesity prevalence in the US has serious public health implications. As rates climb, so do chronic illnesses like type 2 diabetes, hypertension, and cardiovascular disease. This increase puts pressure on healthcare resources, leading to higher costs. According to KFF on healthcare costs, obesity-related conditions add billions to healthcare spending. Hospitals see more admissions for obesity-related illnesses, needing multidisciplinary approaches for complex comorbidities.

Obesity impacts workforce productivity. It leads to more sick days and disabilities. This creates economic burdens for companies. It also worsens health disparities, impacting underserved populations the most. To manage this epidemic, we need strategies that lower cases and boost health for at-risk groups. Community-wide initiatives promoting healthier lifestyles show promise.
Looking Forward: Strategies to Combat the Obesity Epidemic
Addressing the obesity prevalence in the US requires a comprehensive approach. Prevention is key. Teach about balanced diets. Encourage exercise. Build supportive environments. Community programs that promote active living and better access to healthy food can help stop obesity.
Interventions include:
- Expanding healthcare access for screening and counseling.
- Offering behavioral therapies.
- Considering surgical options when needed.
Policy reforms matter. Taxing sugary drinks is important. Limiting unhealthy food ads aimed at kids also helps. Plus, clear nutritional information is essential.
Urban planning that enhances walkability and recreational spaces encourages active lifestyles. Digital health tools—apps and monitoring devices—support ongoing weight management. I focus on health promotion. I believe these strategies can help end obesity and build healthier communities.
Healthy eating and regular exercise remain essential. For actionable ideas, explore articles on the Mediterranean diet and exercise music benefits.
Sources
- Wellness Blogs – 7 Effective Strategies to Embrace Healthy Aging and Thrive in Later Years
- Wellness Blogs – 10 Surprising Physical Education Benefits
- Wellness Blogs – 7 Surprising Hot Water Benefits
- Wellness Blogs – 10 Surprising Benefits of Parks for Physical Activity and Well-Being
- Wellness Blogs – Unlocking the Power of Exercise Music
- Wellness Blogs – Mediterranean Diet Can Improve Your Gum Health


