Understanding Keratoderma Odor: Symptoms, Causes, and Impact
**Search Phrase: Keratoderma odor** is a condition that extends beyond the visible thickening of the skin associated with palmoplantar keratoderma (PPK). A significant yet often overlooked aspect of this condition is the development of a distinctive, unpleasant odor emanating from the affected skin areas. This phenomenon, commonly referred to as **keratoderma odor**, can profoundly impact an individual’s quality of life due to social discomfort and inconvenience.
**Keratoderma odor** is primarily observed in patients with genetic skin conditions like Non-epidermolytic palmoplantar keratoderma (NPPK), a rare disorder characterized by diffuse keratin buildup on the palms and soles. The thickened, fissured skin creates an environment conducive to bacterial colonization. These bacteria metabolize sweat components and skin secretions, producing volatile organic compounds (VOCs) responsible for the characteristic smell associated with keratoderma odor ([NCBI](https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6363212/)).
Individuals with keratoderma odor often notice that the odor worsens with increased sweating or during humid conditions. The presence of persistent cracks and fissures in the thickened skin further traps bacteria and odorous compounds, amplifying the problem. Managing **keratoderma odor** is essential not only for physical comfort but also for social confidence and mental well-being. While there’s no definitive cure, diligent skin care and targeted hygiene can significantly mitigate this unpleasant symptom. For more insights on protecting skin health, consider reading our guide on how to protect your skin barrier in urban environments.
The Role of Skin Bacteria in Keratoderma Odor Among NPPK Patients
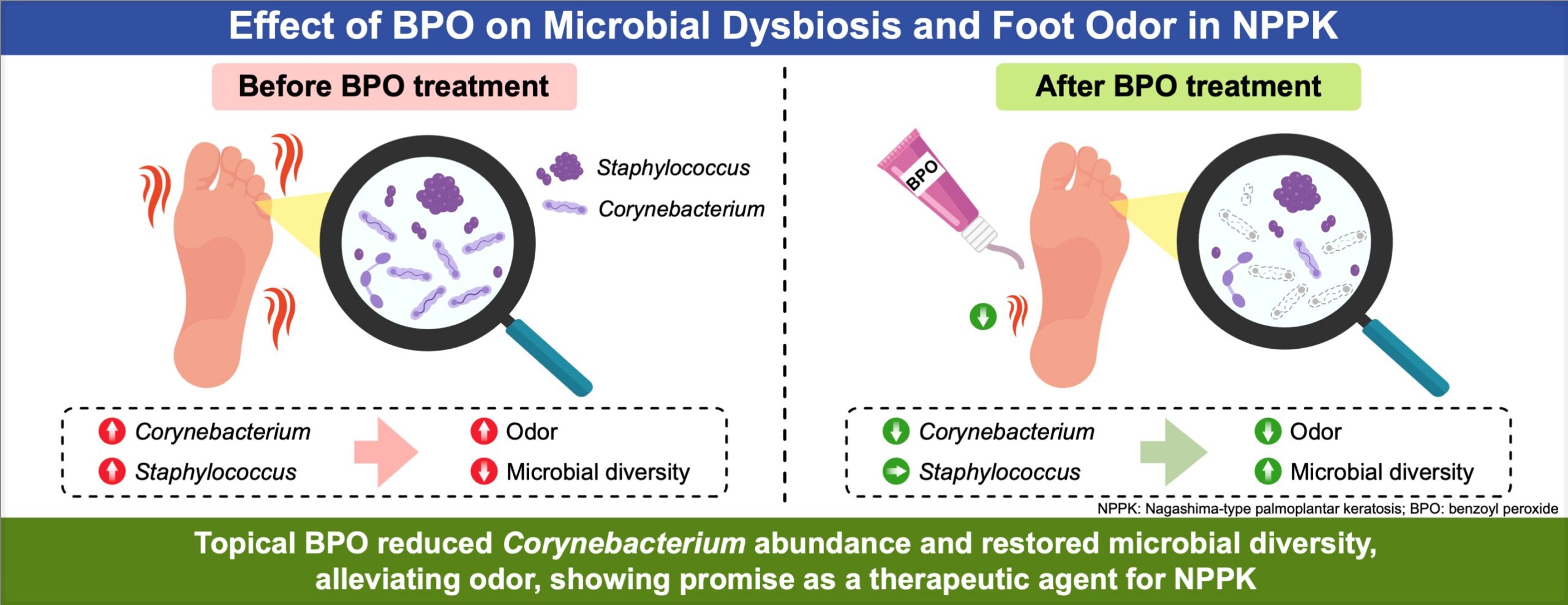
The development of **keratoderma odor** is intricately tied to the microbiome of the skin. In patients with inherited conditions like Nagashima-type palmoplantar keratoderma (NPPK), the hyperkeratotic and fissured skin provides a fertile ground for bacteria such as Corynebacterium and Staphylococcus. These bacteria metabolize sweat and skin secretions like amino acids and lipids, producing malodorous compounds such as isovaleric acid and thioalcohols ([NCBI](https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4997432/)).
Additionally, the thickened skin impairs normal shedding, trapping odor-causing molecules and exacerbating the smell. Proper hygiene, including regular washing and the use of antimicrobial products, can help control bacterial colonization. However, overuse of antimicrobials may disturb the natural balance of skin flora, so a tailored approach is necessary. To learn more about skin microbiota and odor, check out our article on skin microbiota and odor.
Advances in Understanding Keratoderma Odor: Scientific Perspectives
Recent research employing microbiome analysis has enhanced our understanding of **keratoderma odor**. Studies identify specific bacteria, notably Corynebacterium spp., that preferentially colonize thickened, moist skin. These bacteria generate volatile sulfur compounds and other malodorous substances as metabolic byproducts, which are responsible for the distinctive smell ([NCBI](https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7643779/)).
Furthermore, alterations in skin barrier function in keratoderma facilitate bacterial overgrowth, contributing to odor. Advances in personalized topical therapies—such as specific antimicrobials and keratolytic agents—show promise in reducing bacterial load and odor severity ([Dermatology Times](https://pmc.ncbi.nlm.nih.gov/articles/PMC5967208/)). These insights open pathways for more effective management tailored to individual microbiome profiles, improving quality of life for those affected.
Effective Strategies to Manage Keratoderma Odor in NPPK
Controlling **keratoderma odor** involves a combination of diligent hygiene, skin care, and targeted treatments. Here are key practices for managing this challenging symptom:
1. Maintain Rigorous Foot Hygiene
- Wash feet daily with antibacterial soap to reduce bacterial buildup.
- Ensure thorough drying, especially between toes, to minimize moisture conducive to bacteria growth.
2. Use Antiperspirants and Odor Neutralizers
- Apply topical antiperspirants containing aluminum chloride to limit sweating.
- Utilize medicated foot powders that absorb moisture and neutralize odor.
3. Wear Appropriate Footwear and Socks
- Select shoes made of breathable materials like leather or mesh.
- Opt for moisture-wicking socks and change them daily.
4. Apply Topical Treatments
- Keratolytic agents such as salicylic acid can help reduce thickened skin, decreasing bacterial habitat.
- In some cases, clinicians may prescribe antimicrobial creams to diminish bacterial colonization.
5. Incorporate Regular Skin Care Practices
- Gently exfoliate to remove excess keratin and prevent cracks that trap bacteria.
- Use moisturizers suited for keratoderma to maintain skin integrity.
6. Seek Professional Advice
If **keratoderma odor** persists or worsens, consult a dermatologist for tailored treatment plans, potentially involving systemic therapies or specialized procedures. For further guidance on skin barrier protection, examine our article on how to protect the skin barrier in urban environments.
Adopting these strategies can significantly reduce **keratoderma odor**, improving comfort, confidence, and overall quality of life for individuals coping with NPPK.
Sources
- NCBI – Genetic Insights into NPPK
- NCBI – Skin Microbiota and Odor
- NCBI – Advances in Keratoderma Odor Research
- wellnessblogs.in – Microbiome and Keratoderma In-Depth
- wellnessblogs.in – Managing Skin Microbial Interactions
- wellnessblogs.in – Protecting Skin Barrier in Urban Settings
- wellnessblogs.in – Strategies for Foot Odor Control